Asteatotic eczema
background
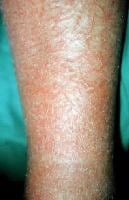
Asteatotic eczema of the lower extremities in elderly persons secondary to aging, dehydrated skin, and malnutrition
Cracked erythema secondary to irritant contact dermatitis from soaps or detergents
Eczema craquelé in areas in which corticosteroid therapy was discontinued
Asteatotic eczema in neurologic disorders
pathophysiology
Initially, excess water loss from the epidermis results in dehydration of the stratum corneum with upward curling of corneocytes. The outer keratin layers require 10-20% water concentration to maintain their integrity. A significant decrease in free fatty acids in the stratum corneum is present in people with asteatotic dermatitis. Stratum corneum lipids act as water modulators, and cutaneous loss of these lipids can increase transepidermal water loss to 75 times that of healthy skin.Elderly persons with decreased sebaceous and sweat gland activity, patients on antiandrogen therapy, people using degreasing agents, and people bathing without replacing natural skin emollients lost to bath water are at risk for asteatotic eczema.
When the stratum corneum loses water, the cells shrink. A significantly decreased cellular volume can stress the skin's elasticity, creating fissures. Edema in the dermis leads to additional stretch on the overlying epidermis. Fissures rupture dermal capillaries, causing clinical bleeding. The disruption of cutaneous integrity can result in inflammation with risk of infection. Transepidermal absorption of allergens and irritants is increased as the epidermis is damaged, increasing susceptibility to allergic contact dermatitis and irritant contact dermatitis.Allergic contact dermatitis and irritant contact dermatitis may cause a persistent and possibly more extensive dermatitis despite therapy. Furthermore, low environmental humidity contributes to xerosis, creating a clinical picture of asteatotic dermatitis in some dermatologic conditions, such as atopic dermatitis.
epidemiology
Men older than 60 years develop asteatotic dermatitis more commonly than women
symptom of asteatotic eczema
- Fissured skin lesions
- Sore skin lesions
- Itchy skin lesions
- Red skin lesions
- Fine cracks in skin
history
The typical presenting picture is an elderly patient complaining of itchy, dry skin in the winter. Younger age groups and even children can, however, be affected. The classical distribution is on the legs, although hands, arms and trunk can also be affected. The appearance is of slightly scaly fissured skin, which has been described as crazy paving or cracked porcelain (see Document reference 2 for a picture). Areas of excoriation, erythema and bleeding may be evident, due to rubbing or scratching. Most patients have a localised condition, but a more severe generalised form is sometimes seen.
. Sometimes, the dysesthesia may be described as a pinprick or biting sensation.
_ Asking the patient about pertinent controllable factors, such as the following, is important:

- Secondary lesions:
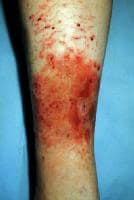
- Excoriated, erythematous, edematous patches may result from rubbing or scratching.
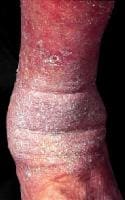
- Bleeding fissures secondary to the disruption of dermal capillaries have been described in exaggerated eczema craquelé, which begins as superficial cracks in the epidermis.
- Xerosis and frictionxerosis: excessive dryness
- Frequent or prolonged bathing in hot water, use of soap on the involved site, and infrequent use of emollients for water retention in the stratum corneum
- Degreasing agents
- Solvents
- Cleansers
- Decreased sebaceous and sweat gland activity in elderly persons
- Decreased keratin synthesis in elderly persons
- Low environmental humidity and cold winds that increase the loss of water by convection
- Radiation
- Long-term malabsorption of essential fatty acids, including linoleic acid and linolenic acid
- Nutritional deficiencies
- Zinc deficiency
- Essential fatty acid deficiency, such as linoleic acid deficiency or linolenic acid deficiency
- Atopy
- Ichthyosis: hereditary skin disease characterized by flaky and scaly skin
- Thyroid disease - Myxedema and other thyroid diseases with diminished sweat and sebaceous gland activity
- Neurologic disorders - Decreased sweating in denervated areas
- Drugs - Antiandrogen therapy and diuretic therapy
- Malignancies - Malignant lymphoma gastric adenocarcinoma, glucagonoma, angioimmunoblastic lymphadenopathy, breast cancer, large-cell lung carcinoma, and colorectal carcinomaDDx
- Cellulitis
- fever not seen in eczema
- Contact Dermatitis, Allergic
- Contact Dermatitis, Irritant
- Stasis Dermatitis
- Thrombophlebitis
histologic finding
Spongiosis and a varying amount of inflammatory dermal infiltrate similar to that of mild, . subacute eczema are seen
inflammation of derm is assosiated with secondary infection
Investigations
- Laboratory tests may be required to exclude associated diseases if clinically suspected.
- Histology of a skin biopsy shows spongiosis (increased intracellular fluid in the epidermis) and some inflammatory dermal infiltrate. These are unfortunately nonspecific findings found in many inflammatory conditions, and the diagnosis is usually made clinically.
treatment and management
Patients should follow the methods listed below to improve the condition.
- Take short baths with decreased water temperature.
- Eliminate or reduce the use of soap on the involved areas.
- Avoid harsh skin cleansers.
- Apply petrolatum-based emollients following bathing, and use moisturizing agents liberally.
- Apply topical steroid ointments with or without polyethylene occlusion. Note that steroids can thin the cutaneous barrier and lower the threshold for further insults that lead to dermatitis, especially in elderly patients.
- Use humidifiers.
- Symptoms can be alleviated by moisturizing and steroid creams. Antibiotics may be needed if secondary infection develops
- Steps for Managing Eczema:
- Make lifestyle changes to avoid temperature, humidity extremes and other exacerbating factors
- Bathe only once every 1-2 days - over-bathing can dry the skin.
- Use bath oil to help moisturise skin e.g. Dermaveen, Hamilton's Alpha Ker or QV
- Keep the nails short and wear a covering over the hands (gloves or socks) to avoid night-time scratching as the patient is often unaware that they are scratching
- Using low-allergenic washing powders
- Wear cotton clothing as other materials increase sweating and rubbing on the skin
- Moisturise twice a day. It may take some experimentation to find a cream that doesn't irritate the skin. Avoid creams with mineral oils. Commonly used brands include: Alpha Keri, Cetaphil, QV, Dermaveen and Hamiltons
- Oils such as olive oil (extra-virgin) may be used as a moisturizer
- A topical cream called Pimecrolimus may be used to treat eczema - it is non-steroidal and doesn't cause thinning of the skin. Strong steroid-based topical creams may be needed for more resistant patches.
- Very red dry skin may benefit from using QV Flare Up Bath Oil
- Use topical antibacterial cream for infected eczema - oral antibiotics may be recommended in more severe cases.
- Avoid environments that are excessively hot, cold or dry as they can exacerbate skin symptoms
- Topical immunomodulators - Pimecrolimus and Tacrolimus - may be used as an alternative to topical steroids
medication summaryTopical steroid ointments with 24- to 48-hour occlusion with polyethylene or Unna boots are the treatment of choice for the rapid resolution of asteatotic dermatitis. Many patients heal with mild topical steroids (class III-VI) alone, depending on the severity of the dermatitis, the patient's compliance with treatment, and the reduction in the use of soap and hot water to the involved areas. Several studies have reported on the successful use of pimecrolimus or tacrolimus cream in conditions other than atopic dermatitis, including seborrheic dermatitis and asteatotic eczema, among others. 4
The liberal use of moisturizers, especially petrolatum-based preparations, alone or in combination with topical steroids for mild cases of asteatotic dermatitis is recommended.
The soak-and-smear method of hydrating the skin by bathing or soaking the affected area followed by immediate application of steroid ointment once daily has been shown to clear more that 90% of patients in 4-14 days. This is best performed at night
Note that steroids can thin the cutaneous barrier and lower the threshold for further insults that lead to dermatitis, especially in elderly patients.
- Use topical antibacterial cream for infected eczema - oral antibiotics may be recommended in more severe cases
- Avoid environments that are excessively hot, cold or dry as they can exacerbate skin symptoms
complication
- Allergy to topical steroids
- Secondary infection
prognosis
Asteatotic dermatitis responds well to therapy; however, if the causative factors are not eliminated, recurrences are common.