Allergic contact dermatitis
backgaround
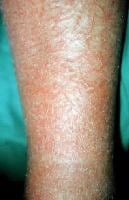
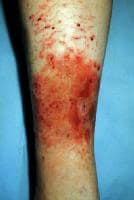
Allergic contact dermatitis (ACD) is a delayed type of induced sensitivity (allergy) resulting from cutaneous contact with a specific allergen to which the patient has developed a specific sensitivity. This allergic reaction causes inflammation of the skin manifested by varying degrees of erythema, edema, and vesiculation.
The term contact dermatitis sometimes is used incorrectly as a synonym for allergic contact dermatitis. Contact dermatitis is inflammation of the skin induced by chemicals that directly damage the skin and by specific sensitivity in the case of allergic contact dermatitis.
A detailed history, both before and after patch testing, is crucial in evaluating individuals with allergic contact dermatitis. Before patch testing, the history identifies potential causes of allergic contact dermatitis and the materials to which individuals are exposed that should be included in patch testing. After patch testing, the history determines the clinical significance of the findings
pathophysiology
Approximately 3000 chemicals are well documented as specific causes of allergic contact dermatitis. Most of the chemicals able to provoke allergic contact dermatitis are small molecules (< 500 d). These molecules must bind to carrier proteins on Langerhans cells, which are situated within the suprabasilar layer of the epidermis.
Langerhans cells are the antigen-presenting cells within the skin. Langerhans cells interact with CD4+ T cells (helper T cells). Skin irritation by both nonallergenic and allergenic compounds induces Langerhans cell migration and maturation. In contrast, only allergenic compounds induce CD1a+ CD83+ Langerhans cell migration with partial maturation at subtoxic concentrations
Cytokines also play an important role in allergic contact dermatitis because they regulate accessory-adhesion molecules, such as intercellular adhesion molecule 1. Interleukin 8 may be a cytokine indicating allergic contact dermatitis, not irritant contact dermatitis.
Langerhans cells can migrate from the epidermis to the regional draining lymph nodes. Sensitization to a chemical requires intact lymphatic pathways.
The initial sensitization typically takes 10-14 days from initial exposure to a strong contact allergen such as poison ivy. Some individuals develop specific sensitivity to allergens following years of chronic low-grade exposure; for example, sensitivity to chromate in cement can eventually develop in individuals with chronic irritant contact dermatitis resulting from the alkaline nature of cement. Once an individual is sensitized to a chemical, allergic contact dermatitis develops within hours to several days of exposure.
CD4+ CCR10+ memory T cells persist in the dermis after clinical resolution of allergic contact dermatitis.
Filaggrin barrier defects that predispose individuals to atopic dermatitis might also predispose them to allergic contact dermatitis by allowing greater penetration of chemical haptens
etiology
Approximately 25 chemicals appear to be responsible for as many as one half of all cases of allergic contact dermatitis. These include nickel, preservatives, dyes, and fragrances.
Poison ivy
Poison ivy (Toxicodendron radicans) is the classic example of acute allergic contact dermatitis in North America. Allergic contact dermatitis from poison ivy is characterized by linear streaks of acute dermatitis that develop where plant parts have been in direct contact with the skin.
Nickel
Nickel is the leading cause of allergic contact dermatitis in the world. The incidence of nickel allergic contact dermatitis in North America is increasing; in contrast, new regulations in Europe have resulted in a decreasing prevalence of nickel allergy in young and middle-aged women
Allergic contact dermatitis to nickel typically is manifested by dermatitis at the sites where earrings or necklaces (see the image below) containing nickel are worn or where metal objects (including the keypads of some cell phones) containing nickel are in contact with the skin.
Nickel may be considered a possible occupational allergen. Workers in whom nickel may be an occupational allergen primarily include hairdressers, retail clerks, caterers, domestic cleaners, and metalworkers. Individuals allergic to nickel occasionally may develop vesicles on the sides of the fingers (dyshidrotic hand eczema or pompholyx) from nickel in the diet.
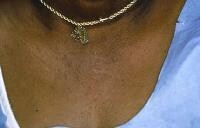 Allergic contact dermatitis to nickel in a necklace.
Allergic contact dermatitis to nickel in a necklace.Rubber gloves
Allergy to 1 or more chemicals in rubber gloves is suggested in any individual with chronic hand dermatitis who wears them, unless patch testing demonstrates otherwise. Allergic contact dermatitis to chemicals in rubber gloves typically occurs maximally on the dorsal aspects of the hand. Usually, a cutoff of dermatitis occurs on the forearms where skin is no longer in contact with the gloves. Individuals allergic to chemicals in rubber gloves may develop dermatitis from other exposures to the chemicals (eg, under elastic waistbands).
Hair dye and temporary tattoos
p-Phenylenediamine (PPD) is a frequent component of and sensitizer in permanent hair dye products and temporary henna tattoos ; exposure in to it in hair dye products may cause acute dermatitis with severe facial edema. Severe local reactions from PPD may occur in black henna tattoos in adults and children. Epidemiologic data indicate that the median prevalence of positive patch test reactions to PPD among dermatitis patients is 4.3% (increasing) in Asia, 4% (plateau) in Europe, and 6.2% (decreasing) in North America.[7]
Textiles
Individuals allergic to dyes and permanent press and wash-and-wear chemicals added to textiles typically develop dermatitis on the trunk, which occurs maximally on the lateral sides of the trunk but spares the vault of the axillae. Primary lesions may be small follicular papules or may be extensive plaques.
Individuals in whom this allergic contact dermatitis is suspected should be tested with a series of textile chemicals, particularly if routine patch testing reveals no allergy to formaldehyde. New clothing is most likely to provoke allergic contact dermatitis, since most allergens decrease in concentration in clothing following repeated washings.
Preservatives
Preservative chemicals added to cosmetics, moisturizers, and topical medications are major causes of allergic contact dermatitis (see the image below). The risk of allergic contact dermatitis appears to be highest to quaternium-15, followed by allergic contact dermatitis to isothiazolinones (Kathon CG). Although parabens are among the most widely used preservatives, they are not a frequent cause of allergic contact dermatitis.
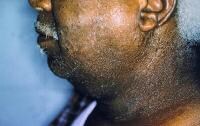 Severe allergic contact dermatitis resulting from preservatives in sunscreen. Patch testing was negative to the active ingredients in the sunscreen.
Severe allergic contact dermatitis resulting from preservatives in sunscreen. Patch testing was negative to the active ingredients in the sunscreen.Schnuch et al estimated that preservatives found in leave-on topical products varied over 2 orders of magnitude in relative sensitization risk.
Formaldehyde is a major cause of allergic contact dermatitis (see the image below). Certain preservative chemicals widely used in shampoos, lotions, other moisturizers, and cosmetics are termed formaldehyde releasers (ie, quaternium-15 [Dowicil 200], imidazolidinyl urea [Germall 115], and isothiazolinones
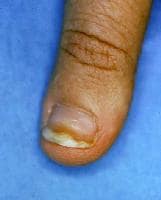 Onycholysis developing from allergic contact dermatitis to formaldehyde used to harden nails.
Onycholysis developing from allergic contact dermatitis to formaldehyde used to harden nails.Fragrances
Individuals may develop allergy to fragrances. Fragrances are found not only in perfumes, colognes, aftershaves, deodorants, and soaps, but also in numerous other products, often as a mask to camouflage an unpleasant odor. Unscented products may contain fragrance chemicals used as a component of the product and not labeled as fragrance.
Individuals allergic to fragrances should use fragrance-free products. Unfortunately, the exact chemicals responsible for a fragrance in a product are not labeled. Four thousand different fragrance molecules are available to formulate perfumes. The fragrance industry is not required to release the names of ingredients used to compose a fragrance in the United States, even when individuals develop allergic contact dermatitis to fragrances found in topical medications.
Deodorants may be the most common cause of allergic contact dermatitis to fragrances because they are applied to occlude skin that is often abraded by shaving in women.
Massage and physical therapists and geriatric nurses are at higher risk of occupational allergic contact dermatitis to fragrances.
Corticosteroids
In the last decade, it has become clear that some individuals with chronic dermatitis develop allergy to topical corticosteroids. Most affected individuals can be treated with some topical corticosteroids, but an individual can be allergic to all topical and systemic corticosteroids. Budesonide and tixocortol pivalate are useful patch test corticosteroids for identifying individuals allergic to topical corticosteroids.
Neomycin
The risk of allergy to neomycin is related directly to the extent of its use in a population. The risk of allergy to neomycin is much higher when it is used to treat chronic stasis dermatitis and venous ulcers than when it is used as a topical antibiotic on cuts and abrasions in children. Assume that individuals allergic to neomycin are allergic to chemically related aminoglycoside antibiotics (eg, gentamicin, tobramycin).Avoid these drugs both topically and systemically in individuals allergic to neomycin.
Benzocaine
Avoid topical use of benzocaine. Benzocaine is included in most standard patch test trays. Individuals allergic to benzocaine may safely use or be injected with lidocaine (Xylocaine), which does not cross-react with benzocaine.
Many individuals complain of adverse reactions to sunscreens, but many of these individuals are not allergic to the sunscreen materials. They may be allergic to preservatives in these products or may have nonspecific cutaneous irritation from these products.
Photoallergy
Occasionally, individuals develop photoallergic contact dermatitis. Allergic contact dermatitis may be accentuated by ultraviolet (UV) light, or patients may develop an allergic reaction only when a chemical is present on the skin and when the skin is exposed sufficiently to ultraviolet light A (UV-A; 320-400 nm).
epidemiology
No racial predilection exists for allergic contact dermatitis. Allergic contact dermatitis is more common in women than in men. This predominantly is a result of allergy to nickel, which is much more common in women than in men in most countries.
Allergic contact dermatitis may occur in neonates. In elderly individuals, the development of allergic contact dermatitis may be delayed somewhat, but the dermatitis may be more persistent once developed. Contact allergy to topical medicaments is more common in persons older than 70 years
prognosis
Individuals with allergic contact dermatitis may have persistent or relapsing dermatitis, particularly if the material(s) to which they are allergic is not identified or if they continue to practice skin care that is no longer appropriate (ie, they continue to use harsh chemicals to wash their skin, they do not apply creams with ceramides or bland emollients to protect their skin).
The longer an individual has severe dermatitis, the longer it is believed it will take the dermatitis to resolve once the cause is identified.
Some individuals have persistent dermatitis following allergic contact dermatitis, which appears to be true especially in individuals allergic to chrome.
A particular problem is neurodermatitis (lichen simplex chronicus), in which individuals repeatedly rub or scratch an area initially affected by allergic contact dermatitis.
Mortality
Death from allergic contact dermatitis is rare in the United States. Allergic contact dermatitis to the weed wild feverfew caused deaths in India when the seeds contaminated wheat shipments to India. This plant then became widespread and a primary cause of severe airborne allergic contact dermatitis.
history
A detailed history, both before and after patch testing, is crucial in evaluating individuals with allergic contact dermatitis. Potential causes of allergic contact dermatitis and the materials to which individuals are exposed should be included in patch testing. Evaluation of allergic contact dermatitis requires a much more detailed history than most other dermatologic disorders.
History is equally important after patch testing. Only history and questioning can determine whether the materials to which a patient is allergic are partly or wholly responsible for the current dermatitis. A positive patch reaction may indicate only a sensitivity and not the cause of current dermatitis.
Preexisting skin diseases
Individuals with stasis dermatitis are at high risk for developing allergic contact dermatitis to materials and agents applied to the areas of stasis dermatitis and leg ulcers. Neomycin is an important cause of allergic contact dermatitis in these individuals because it is used frequently despite the lack of documentation of its efficacy in the treatment of stasis ulcers.
Individuals with otitis externa frequently are allergic to topical neomycin and topical corticosteroids.
Individuals with pruritus ani and pruritus vulvae may become sensitized to benzocaine and other medications applied to chronic pruritic processes.
Women with lichen sclerosus et atrophicus frequently develop allergic contact dermatitis, complicating the severe chronic vulvar dermatosis. Patch testing these patients may provide important information that can help in the management of recalcitrant and difficult-to-manage dermatosis.
Atopic dermatitis
Patients with a history of atopic dermatitis are at increased risk for developing nonspecific hand dermatitis and irritant contact dermatitis. However, they do not appear to be at an increased risk for allergic contact dermatitis, despite the wide range of topical medications and moisturizers used by individuals with chronic atopic dermatitis. They are at lower risk of allergic contact dermatitis to poison ivy. Some European studies indicate that patients with atopic dermatitis may have increased incidence of allergic contact dermatitis to nickel.
Onset of symptoms
Individuals with allergic contact dermatitis typically develop dermatitis, within a few days of exposure, in areas that were exposed directly to the allergen. Certain allergens (eg, neomycin) penetrate intact skin poorly, and the onset of dermatitis may be delayed up to a week following exposure.
A minimum of 10 days is required for individuals to develop specific sensitivity to a new contactant. For example, an individual who never has been sensitized to poison ivy may develop only a mild dermatitis 2 weeks following the initial exposure but typically develops severe dermatitis within 1-2 days of the second and subsequent exposures.
Remember that removing the poison ivy allergen from the skin is difficult, and unless an individual washes exposed skin within 30 minutes of exposure, allergic contact dermatitis will develop. The hallmark of the diagnosis of poison ivy is linear dermatitic lesions. The possibility of an external cause of dermatitis always must be considered if the dermatitis is linear or sharply defined.
The immediate onset of dermatitis following initial exposure to material suggests either a cross-sensitization reaction, prior forgotten exposure to the substance, or nonspecific irritant contact dermatitis provoked by the agent in question.
Eyelid dermatitis
Individuals may develop dermatitis on eyelids and other exposed skin following exposure to airborne allergens or allergens transferred to that site by the fingers. Contact dermatitis may also result from allergy to eyelid makeup.
Contact urticaria
Immediate reactions, ie, visible lesions developing less than 30 minutes after exposure, indicate contact urticaria (not allergic contact dermatitis). This is particularly true if the lesions are urticarial in appearance and if the skin reaction is associated with other symptoms, such as distant urticaria, wheezing, ophthalmedema, rhinorrhea, or anaphylaxis.
Latex
Rubber latex currently is the most important source of allergic contact urticaria (see Latex Allergy). The term hypoallergenic may refer to gloves that do not contain sensitizing chemicals added to rubber latex but may not indicate whether the gloves are rubber latex free.
Some individuals may have delayed specific contact sensitivity to rubber latex, but contact urticaria to rubber latex is much more common than allergic contact dermatitis to latex. Individuals with hand dermatitis, hospital workers, children with spina bifida, and atopic individuals are at increased risk of developing contact urticaria to rubber latex. Individuals may have allergic contact dermatitis to chemicals added to rubber gloves and have contact urticaria to latex. Individuals wearing rubber gloves should be evaluated carefully for both possibilities.
Rare reports exist of immediate anaphylactic reactions to topical antibiotics (eg, bacitracin).
Occupational dermatitis
Contact dermatitis is 1 of the 10 leading occupational illnesses. It may prevent individuals from working. The hands are the sites exposed most intensely to contact allergens and irritants, both at work and at home. Allergic contact dermatitis in response to workplace materials may improve initially on weekends and during holidays, but individuals with chronic dermatitis may not demonstrate the classic history of weekend and holiday improvement.
Irritant contact dermatitis is more likely if multiple workers are affected in the workplace. Most allergens rarely sensitize a high percentage of the population.
Hobbies
Hobbies may be the source of allergic contact dermatitis. Examples include woodworking with exotic tropical woods or processing film using color-developing chemicals that may provoke cutaneous lesions of lichen planus from direct skin exposure.
Medications
Medications (both self-prescribed and physician-prescribed) are important causes of allergic contact dermatitis. The workplace nurse may dispense ineffective and sensitizing topical preparations, such as thimerosal (Merthiolate), which may change a simple abrasion into a severe case of allergic contact dermatitis. Individuals may develop allergy to preservatives in medications and/or to the active ingredients in topical medications, especially neomycin and topical corticosteroids.[11, 12]
Patients with dermatitis that did not clear with topical corticosteroid treatment should be considered for patch testing with a corticosteroid series and the commercial preparations of corticosteroids and their vehicles.
physical examination
Acute allergic contact dermatitis is characterized by pruritic papules and vesicles on an erythematous base. Lichenified pruritic plaques may indicate chronic allergic contact dermatitis. Occasionally, allergic contact dermatitis may affect the entire integument (ie, erythroderma, exfoliative dermatitis). The initial site of dermatitis often provides the best clue regarding the potential cause of allergic contact dermatitis. Note the following.
Hands
Hands are an important site of allergic contact dermatitis, particularly in the workplace. Common causes of allergic dermatitis on the hands include the chemicals in rubber gloves.
Topical medication sites
Allergic contact dermatitis is frequent in the perianal area as a result of the use of sensitizing medications and remedies (eg, topical benzocaine). Topical medications are also important causes of allergic contact dermatitis in cases of otitis externa. Allergy to chemicals in ophthalmologic preparations may provoke dermatitis around the eyes.
Airborne allergic contact dermatitis
Chemicals in the air may produce airborne allergic contact dermatitis. This dermatitis usually occurs maximally on the eyelids, but it may affect other areas exposed to chemicals in the air, particularly the head and the neck.
Hair dyes
Hair dye—in particular, the component p-phenylenediamine (PPD)—may trigger allergic contact dermatitis. Individuals allergic to hair dyes typically develop the most severe dermatitis on the ears and adjoining face rather than on the scalp.
Stasis dermatitis and stasis ulcers
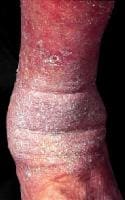
Individuals with stasis dermatitis and stasis ulcers are at high risk for developing allergic contact dermatitis to topical medications applied to inflamed or ulcerated skin (see the image below). The chronicity of this condition and the frequent occlusion of applied medications contribute to the high risk of allergic contact dermatitis to medicament (eg, neomycin) in these patients.
Individuals may develop widespread dermatitis from topical medications applied to leg ulcers or from cross-reacting systemic medications administered intravenously. For example, a patient allergic to neomycin may develop systemic contact dermatitis if treated with intravenous gentamicin.
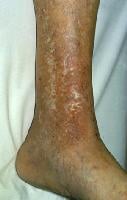 Chronic stasis dermatitis with allergic contact dermatitis to quaternium-15, a preservative in moisturizer. Allergic contact dermatitis produces areas of erythema in areas of atrophie blanche and varicose veins.
Chronic stasis dermatitis with allergic contact dermatitis to quaternium-15, a preservative in moisturizer. Allergic contact dermatitis produces areas of erythema in areas of atrophie blanche and varicose veins.Erythema multiforme
Erythema multiforme (EM) is a severe cutaneous reaction with targetoid lesions that occurs primarily after exposure to certain medications or is triggered by infection, most commonly by herpes simplex virus. Rare cases of EM have been reported after allergic contact dermatitis resulting from exposure to poison ivy,[13]tropical woods, nickel, and hair dye (see the image below).
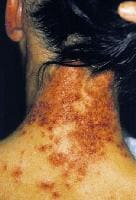 Erythema multiformelike reaction that developed acutely following hair dying.
Erythema multiformelike reaction that developed acutely following hair dying.Intraoral metal contact allergy may result in mucositis that mimics lichen planus, which has an association with intraoral squamous cell carcinoma. Intraoral squamous cell carcinoma adjacent to a dental restoration containing a metal to which the patient was allergic has been reported.[14]
Allergic contact dermatitis may be a direct trigger for skin ulceration in patients with venous insufficiency. Early diagnosis and treatment of allergic contact dermatitis may prevent the development of venous ulcers.
Complications
Darkly pigmented individuals may develop areas of hyperpigmentation or hypopigmentation from allergic contact dermatitis. Occasionally, they may develop depigmentation at sites of allergic contact dermatitis to certain chemicals.
Occasionally, allergic contact dermatitis is complicated by secondary bacterial infection, which may be treated by the appropriate systemic antibiotic.
DDx
- Asteatotic Eczema
- Contact Dermatitis, Irritant
- Drug-Induced Bullous Disorders
- Drug-Induced Photosensitivity
- Nummular Dermatitis
- Onycholysis
- Perioral Dermatitis
- Phytophotodermatitis
- Prurigo Nodularis
- Seborrheic Dermatitis
- Tinea Corporis
- Transient Acantholytic Dermatosis
- Urticaria, Contact Syndrome
lab studies
Potassium hydroxide preparation and/or fungal culture to exclude tinea are often indicated for dermatitis of the hands and feet. This will identify disorders such astinea pedis.
histologic finding
The histology of allergic contact dermatitis is similar to that found in other forms of eczematous dermatitis. A pattern of subacute chronic dermatitis or acute dermatitis may be seen. The inflammatory infiltrate in the dermis predominately contains lymphocytes and other mononuclear cells.
Epidermal edema (ie, spongiosis and microvesicle formation) may be seen, but these changes may be absent in long-standing dermatitis in which thickening of the epidermis (acanthosis) with hyperkeratosis and parakeratosis may be seen in the epidermis and stratum corneum. Allergic contact dermatitis may provoke atypical T-cell infiltrates, simulating mycosis fungoides.