Section 3: Connective Tissue
The connective tissues include a variety of cells, non-living cell products, and blood. A classification and a concise discussion of the various connective tissues follows.
- Adult Connective Tissue
Connective Tissue Proper
The loose or areolar connective tissue is made up of many cell types and intercellular materials (matrix), which also comprise other connective tissues but in varying proportions. It is widely distributed in the body and is found most readily beneath the skin and superficial fascia (fatty connective tissue), separating muscles, in all potential spaces, and beneath the epithelial lining in the lamina propria of the digestive system. This web-like tissue binds cells and organs together but permits these cells and organs to move, as necessary, in relation to each other. Because it is composed of a large amount of amorphous ground substance (whose consistency varies from liquid to gel), it allows wandering cells to move around freely and other structures, such as blood vessels and nerve, to pass through it. This connective tissue is important, because of its cellular content, for defense against infection and the repair of damaged tissue
Important cells found in the loose connective tissue include the following: Fibroblasts, which synthesize collagenous connective tissue fibers that are flexible but of great tensile strength; macrophages (or histiocytes) and monocytes, which ingest, digest, or "store" microscopic particles such as debris of dead cells; certain microorganisms; and other non-biodegradable matter. Capable of ameboid movement, these cells wander throughout the connective tissue and congregate in regions requiring their specialized function. Mast cells synthesize and release substances of physiological importance (e.g., heparin and histamine).
Heparin is a powerful anticoagulant of blood, whereas histamine increases the permeability of blood capillaries. Circulating eosinophils increase in number in parasitic infections and in hypersensitivity reactions, such as in hay fever and asthma. Factors within the specific granules of eosinophils are thought to function as anti-larval agents in helminthic infections; additional factors can be directed against histamine and other inflammatory agents. Lymphocytes and plasma cells also populate loose connective tissue and play a vital role in the defense mechanism by producing antibodies, the immunoglobulins of the blood. Eosinophils, lymphocytes, and plasma cells are particularly abundant in the lamina propria of the digestive system and other potentially vulnerable areas of the body.
In the digestive system and elsewhere, the individual is separated from pathogenic organisms of the external environment by only a delicate single cell layer. This cell layer is essential for absorption, excretion, and gaseous exchange; it is therefore vital to maintain defensive cells just below the vulnerable surface. Fat cells may occur singly or in small or large numbers. When fat cells predominate, the tissue is called adipose tissue. One of the special connective tissues, adipose tissue, serves as a reservoir of energy and as a soft packing in potential spaces (e.g., axilla and ischiorectal fossa) and for organs. It also envelopes glands that undergo cyclic or functional variation in size and activity (e.g., mammary glands), surrounds mobile organs (e.g., eye and heart), and protects other organs (e.g., kidney), blood vessels, and nerve fiber bundles.
The more important intercellular components of the loose connective tissue include three kinds of fibers (collagenous, previously mentioned, and elastic and reticular) and amorphous ground substance. Collagenous and reticular fibers belong to the same class of protein, collagen, whereas elastic fibers are formed of elastin. There are many kinds of collagen, and it is the most abundant protein of the human body (about 30 percent of the dry weight). Ground substance is composed primarily of two classes of compounds: glycosaminoglycans and structural glycoproteins. The term glycosaminoglycan is replacing the older, but widely used, term mucopolysaccharide to denote a linear polysaccharide with characteristic repeating disaccharide units. The repeating units are usually a uronic acid and a hexosamine. The uronic acid may be glucuronic or iduronic acid, and the hexosamine may be glucosamine or galactosamine. The structural glycoproteins play an important role in cell interaction and in migration and adhesion of cells. Fibronectin, laminin, and chondronectin are three structural glycoproteins; these cannot, however, be distinguished by routine histological techniques. It might be useful to remember, as you review your microscope slides and the photomicrographs in this book, that collagenous fibers are acidophilic and therefore stain red with eosin, stain blue with Mallory's trichrome, and stain green with Masson's trichrome. Elastic fibers may or may not stain well with eosin or Masson's stain, and they may or may not stain (red or yellow) with Mallory's stain; however, old elastic fibers will stain better than younger elastic fibers. Elastic fibers do stain well with toluidine blue (often used to stain 1 µm plastic-embedded tissues) , aldehyde fuchsin orcein phosphotungstic acid hernatoxylin and Weigert's elastic tissue stain .Reticular fibers are argyrophilic and therefore stain with silver stains such as Wilder's method. Ground substance or basement membrane is stained by aldehyde fuchsin periodic acid-Schiff stain and toluidine blue
Dense connective tissue contains fewer cells, but, when they are present, they are similar in type to those found in loose connective tissue. Collagenous (Type 1) fibers predominate in this type of connective tissue. Dense connective tissue appears in two forms: dense irregular and dense regular connective tissue. The irregular type is found in the dermis of the skin, deep fascia surrounding and defining muscles, capsules of organs, and nerve sheaths. Dense regular connective tissue is found mainly in ligaments and tendons , which provide flexible but inelastic unions between bones and between bones and skeletal muscle. At low magnification, a tendon may be confused with striated muscle, because the fibers are axially arranged and the alignment of fibroblast nuclei resembles that found in striated muscle. At higher magnifications, however, the structural differences are easily recognized and a proper identification is readily accomplished. Other examples of dense regular connective tissue include most ligaments, aponeuroses, and the cornea of the eye
Connective tissues with special characteristics of structure and function include elastic, reticular, and pigmented types. Adipose tissue, which also belongs to this group, has already been mentioned and will be indelibly remembered by students of gross anatomy as the layer of tissue immediately below the skin. The fatty tissue is also known as superficial fascia or as the panniculus adiposus. Adipose tissue is of two types: white, "signet ring," unilocular fat , which is ubiquitous; and brown, multilocular, fat , which is uncommon in the adult human.
Elastic fibers in dense parallel bands (elastic tissue) can be found associated with the vertebral column (ligamenturn flava), the suspensory ligament of the penis, and vocal cords. The fascia of the lower anterior abdominal wall (Scarpa's fascia) is predominantly elastic tissue. Elastic fibers are obviously functionally important components of skin and hollow organs, including elastic arteries of the vascular system , trachea and bronchi of the respiratory system, and others. Reticular fibers are composed of collagen (Type 3) and are very fine and highly branched. They form supporting networks around blood vessels and cells in some organs. They are in continuity with other collagenous fibers; they are also inelastic. These fibers are only revealed by special histological techniques . Reticular fibers are found in abundance in lymph nodes, blood-forming organs, spleen, liver, and elsewhere, but, as mentioned previously, they cannot be seen unless special methods using silver salts are used to reveal their presence. This type of connective tissue is associated with phagocytic reticular cells, for example, the reticular cells of lymph nodes and Kupffer's cells of the liver . Pigment tissue is a cellular connective tissue rather than a fibrous non-living connective tissue and has many melanin-containing connective tissue cells. It is found principally in the choroid and iris of the eye
Cartilage
Cartilage is a non-vascular tissue containing fibrous connective tissue (collagen Type 2) embedded in an abundant and firm matrix. The cells that produce cartilage are called chondroblasts, and, in mature cartilage where the cells are housed in lacunae, they are termed chondrocytes. In early development, the greater part of the skeleton is cartilaginous, but, during later stages of development, the cartilage is remodeled and replaced by bone. The process is called endochondral ossification. Three types of cartilage are recognized: hyaline, elastic, and fibrocartilage. Hyaline cartilage is found at the ventral ends of ribs and in the nose, larynx, trachea, and articular surfaces of adjacent bones of movable joints. The matrix or ground substance of cartilage is strongly basophilic and stains metachromatically with toluidine blue and other similar basic dyes . It is the acidic sulfate groups of the proteoglycans comprising the ground substance that account for the staining reaction just noted. Metachromasia means that a cell or tissue takes on a color different from the dye solution with which it is stained.
Fibrocartilage has a limited distribution. It is found in the intervertebral discs, pubic symphysis, menisci and ligaments of the knee and other joints, and in the tendons of some muscles where they glide over bones (e.g., tendons of peroneus longus and tibialis posterior. Fibrocartilage is composed predominantly of collagenous (Type 1) fibers arranged in bundles, with cartilage cells surrounded by a sparse cartilage matrix between the fibrous bundles. Fibrocartilage has characteristics similar to both dense connective tissue and hyaline cartilage. It is always associated with dense connective tissue, and, because of its usual paucity of cartilage cells, there appears to be a gradual transition between the two types of connective tissue. Although cartilage cells are not abundant, they are arranged in scattered clusters in parallel arrays, reflecting the direction of stresses placed upon the tissue. Fibrocartilage has no identifiable perichondrium and differs in this regard from hyaline and elastic cartilage. Elastic cartilage is found in the external ear (pinna), auditory tube, epiglottis, and corniculate and cuneiform cartilages of the larynx . It is yellow and is more flexible and elastic than the other cartilage types owing to abundant branching elastic fibers in its matrix. Elastic fibers are often concentrated in the walls of lacunae, which house cartilage cells.
Bone
Bone is a tissue that forms the greatest part of the skeleton and is one of the hardest structures of the body. It is the rack upon which all the soft parts are suspended or attached. Only the dentin and enamel of teeth are harder. The skeleton is tough and slightly elastic, withstanding tension and compression. Bone differs from cartilage by having its collagenous connective tissue matrix impregnated with organic salts (primarily calcium phosphate and lesser amounts of calcium carbonate, calcium fluoride, magnesium phosphate, and sodium chloride). The osteoblasts, which form the osseous tissue , become encapsulated in lacunae but maintain contact with the vascular system via microscopic canaliculi . When they become encapsulated, they are referred to as osteocytes.
A characteristic feature of a cross section of the shaft (diaphysis) of a long bone is its organization in concentric rings around a central canal containing a blood vessel. This is called a Haversian system (osteon). Between neighboring Haversian systems are non-concentric lamellae, devoid of Haversian canals, termed interstitial lamellae. Vascular canals, called Volkmann's canals , traverse the long axis of the bone; they are always at right angles to Haversian canals. Their function is to link vascular canals of adjacent Haversian systems with each other and with the periosteal and endosteal blood vessels of the bone. The outer perimeter of a long bone, beneath the osteogenic connective tissue (called periosteum), is composed of circumferential lamellae, which also lack Haversian canals. This thick-walled hollow shaft of compact bone (the diaphysis) contains bone marrow. At the distal ends of long bones, where Haversian systems are not found, the bone appears spongy and is therefore called cancellous, or spongy, bone. The spongy appearance is misleading, because careful examination of the architecture reveals a highly organized trabecular system providing maximal structural support with minimal density of bony tissue. The epiphyses at the ends of the diaphysis or shaft contain the spongy bone covered by a thin layer of compact bone. The cavities of the epiphyseal spongy bone are in contact with the bone marrow core of the diaphysis except during growth of long bones in young animals. Interposed between the epiphysis and the diaphysis is the cartilaginous epiphyseal plate. The epiphyseal plate is joined to the diaphysis by columns of cancellous bone; this region is known as the metaphysis.
When bone is formed in and replaces a cartilaginous "model," the process is termed endochondral ossification. Some parts of the skull develop from osteogenic mesenchymal connective tissue, however, without a cartilaginous "model" having been formed first. This is termed intramembranous ossification, and these bones are called membrane bones. In both instances, three types of cells are associated with bone formation, growth, and maintenance: osteoblastsosteocytes and osteoclasts .The osteoblasts produce osseous tissue (bone), become embedded in the matrix they manufacture, and are then renamed osteocytes, to reflect their change of status. They remain viable, because they have access to the vascular supply via microscopic canaliculi through which cellular processes extend to receive nutrients and oxygen. Osteoclasts actively resorb and remodel bone as required for growth; these are giant, multinuclear, phagocytic, and osteolytic cells.
Blood and Lymph
This type of connective tissue is peculiar because its matrix is liquid. The blood is carried in blood vessels and is moved throughout the body by the contractile power of the heart. Blood vessels and heart are discussed in Section 8 of this book. Lymph is found in lymph vessels but originates in extracellular spaces as extracellular fluid, which is normally extravasated from blood capillaries. The extracellular fluid, which enters the lymphatic system of vessels, will have mononuclear white blood cells added to it as the fluid is filtered through lymph nodes, which produce such cells. Lymph is returned to the blood stream near the right and left venous angles junction of the internal jugular and subclavian veins). The lymphatic system is discussed more fully in Section 9.
Mesenchyme
Derived from embryonic mesoderm, mesenchyme is the first connective tissue formed. The cells are widely spaced, with an abundance of intercellular matrix. The primitive mesenchymal cells differentiate into all the supporting tissues of the body. The cells derived from the mesenchyme include blood cells, megakaryocytes, endothelium, mesothelium, reticular cells, fibroblasts, mast cells, plasma cells, special phagocytic cells of the spleen and liver, cartilage cells, and bone cells as well as smooth muscle.
Mucoid Tissue
Widely distributed in the embryo as a loose connective tissue, mucoid tissue is composed of large stellate fibroblasts in an abundant intercellular substance, which is homogeneous and soft. In the umbilical cord it is known as Wharton's jelly.
Subcutaneous
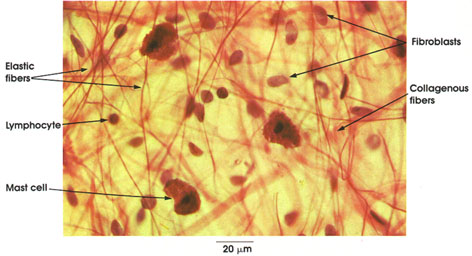
Areolar connective tissue is so-named because of the many small areas or potential spaces that are seen within this tissue. It is the most widely encountered type of connective tissue and contains most of the connective tissue components.
Collogenous fibers: Coarse interlacing bundles of fibers that run in all directions in the connective tissue.
Elastic fibers: Slender network of branching fibers irregularly dispersed in the connective tissue. Smaller than the collagen fiber bundles.
Mast cell: A large cell with a small spherical nucleus and abundant cytoplasm containing coarse granules. Produces heparin and histamine. In some animals, 5-hydroxytryptamine (serotonin) is also produced by this cell.
Fibroblasts: Only nuclei are seen in this preparation. Nuclei are ovoid and larger than other connective tissue nuclei. Fibroblasts are the most common cell type found in areolar connective tissue. They synthesize and deposit collagen.
Lymphocyte: Only nuclei are seen in this preparation. Smaller than fibroblast nuclei, rounder and more deeply stained. They are not as abundant as fibroblasts.
MAST CELLS
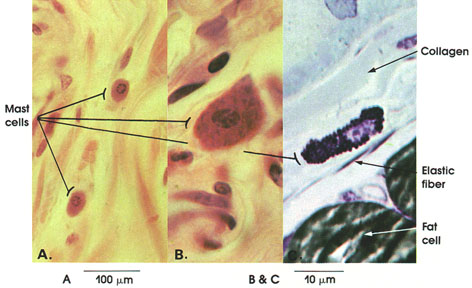
A. Human, 10% formalin, H. & E., 162 x.
B. Rat, Helly's fluid, toluidine blue and erythrocin stains, 1416 x.
C. Rat, glutaraldehyde-osmium fixation, toluldine blue stain, 1416 x.
Mast cells are found in areolar connective tissue and along the course of small blood vessels. They have a spheroid nucleus and abundant cytoplasm. The cytoplasm is filled with coarse granules that stain red in H. & E. preparations (A), but stain metachromatically with toluidine blue and other basic aniline dyes (B and C). Granules may be so abundant as to obscure the nucleus.
In man, mast cells produce heparin, an anticoagulant substance that prevents blood clots. They also produce histamine, which increases the permeability of capillaries and influences the blood pressure.
In rats, mast cells also contain serotonin (5-hydroxytryptamine), which causes vasoconstriction and elevation of blood pressure.
Collagen and elastic fibers are scattered in the interstices between mast cells. Two fat cells stained black by osmium tetroxide fixation are seen in C.
Lamina propria
jejunum
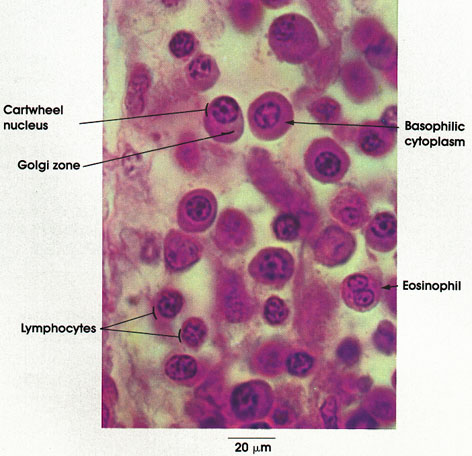
Plasma cells, although uncommon in loose connective tissue, are plentiful in the lamina propria of the digestive tract. Note the ovoid shape of the cell, the eccentric round or oval nucleus, and the intensely basophilic cytoplasm. The less densely stained area of the cytoplasm in juxtaposition to the nucleus contains the Golgi complex and centrioles. Nuclear chromatin is characteristically clumped around the periphery of the nucleus and produces, in negative image, a radial pattern resembling the spokes of a wheel. The basophilia of the cytoplasm is shown by electron microscopy to be due to an extensive system of membrane-bound ribonucleoprotein. These cells produce antibodies.
Note the bilobed nucleus characteristic of human eosinophils in loose connective tissue. Eosinophils reach the lamina propria from the blood capillaries. The coarse, intensely eosinophilic
Compare the size of lymphocytes and plasma cells. Note that the nucleus of the lymphocyte fills most of the cell, with only a thin rim of basophilic cytoplasm around it. Some of the lymphocytes in the lamina propria migrate through the epithelium to the lumen, where they are eliminated.
Lung
terminal bronchiole
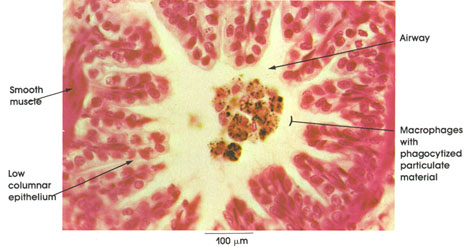
This illustration shows a cross section of a terminal bronchiole with phagocytized material (black) in macrophages within the lumen of the bronchiole (airway). The pleating of the epithelial lining denotes a constricted bronchiole. Note the low columnar epithelial lining of the wall of the bronchiole and the smooth muscle bundle adjacent to the lining epithelium.
Embryonic triceps muscle tendon
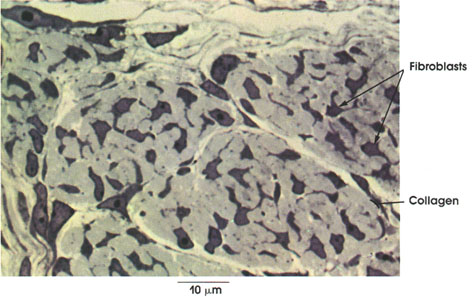
Fibroblasts: Also known in mature tendons as tendon cells, or fibrocytes, they are the only cell type present. They are stellate in shape with cytoplasmic processes extending between and around the collagen bundles.
Collagen: In thick bundles or fascicles, separated by tendon cells and loose connective tissue. Collagenous connective tissue fibers are protein and synthesized by fibroblasts
Tendo calcaneus (tendon of Achilles)
longitudinal section
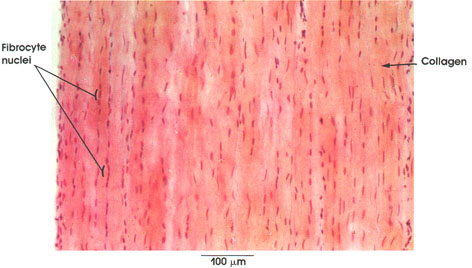
Tendons may be confused with striated muscle sections. This confusion can be avoided by examining the tissue at higher magnifications, where the presence or absence of cross striations will be diagnostic.
Collagen: Fibers oriented in one direction and in dense aggregates and bundles separated by a small amount of areolar connective tissue containing vessels and nerves. Collagen fibrils are flexible, have high tensile strength, and are inelastic. This large tendon links the gastrocnemius and soleus muscles with the calcaneus bone at the rear of the foot.
Fibrocyte nuclei: The predominant cell in this type of connective tissue (dense collagenous type) is oriented primarily in the longitudinal axis, in rows between the bundles of collagenous fibers.
Temporal bone and stapes
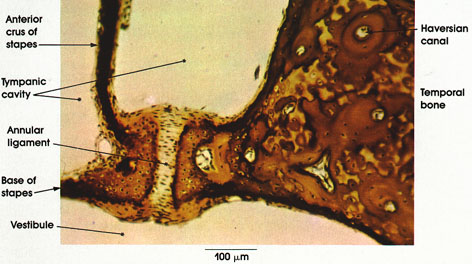
Tympanic cavity: Air-containing space in the middle ear. Limited laterally by the tympanic membrane and medially by the osseous labyrinth. Although not illustrated here, the cavity contains the chorda tympani nerve, the auditory ossicles, and the small tendons of the stapedius and tensor tympani muscles, which are connected to the bony ossicles.
Stapes: One of the three auditory ossicles in the tympanic cavity. It was so-named by the Italian anatomist, Ingrassias, who described it in 1546. The name is derived from Latin (stare, to stand; pes, foot; the thing in which the foot stands) because of its resemblance to a stirrup. The ossicle consists of a head, neck, two limbs, or crura, and a base. The two crura are connected to the base. This figure shows only the anterior crus of the stapes and part of the base.
Anterior crus of stapes: Shorter and less curved than the posterior crus with which it is connected by the base.
Base of stapes: Also called foot plate of the stapes. Fixed to the margin of the fenestra vestibuli (ovalis) by the annular ligament. Also connects the two crura of the stapes.
Annular ligament: A ring of fibroelastic tissue that fixes the base of the stapes to the fenestra vestibuli but permits the stapes to rock or move in response to vibrations of the eardrum. The sound waves are transmitted to the stapes by the incus and malleus (the other two auditory ossicles).
Vestibule: Large bony cavity medial to the tympanic cavity. In its lateral wall is the fenestra vestibuli, to which the foot of the stapes is fixed.
Temporal bone: Surrounding the ear cavities and containing the vestibular and sound receptor organs (semicircular canals and the cochlea
COLLAGENOUS FIBERS
Aorta
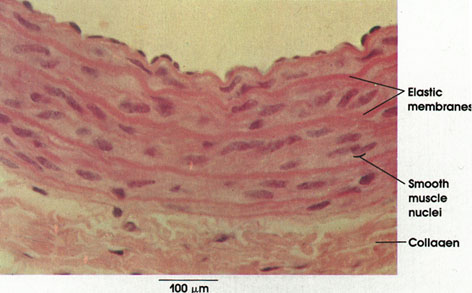
The general method used in this preparation allows differentiation of the various vessel wall components only by the variations in the intensity of staining. The pronounced eosinophilia of the elastic fibers reflects their high content of basic amino acids. .
Elastic membranes: Abundant in the media of elastic arteries. The elastic fibers anastomose to form a fenestrated "membrane," which is circularly arranged in layers.
Smooth muscle nuclei: Smooth muscle fibers are located between the elastic fiber networks. Circularly disposed.
Collagen: In the adventitia, collagen forms a loose irregular connective tissue layer surrounding the blood vessel. Elastic fibers, not distinguishable by this method, are also found in this connective tissue coat.
COLLAGENOUS FIBERS
Aorta
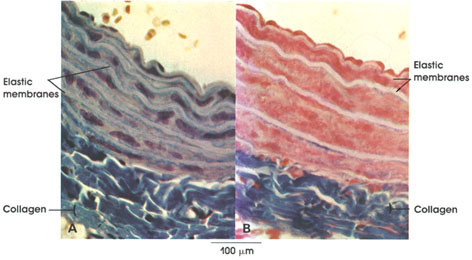
Mallory-azan stain (B), 162 x.
Elastic membranes: Elastic membranes are a striking feature of the aorta. Located within the tunica media of the vessel wall, they serve as "shock absorbers." Elastic arteries are subject to the greatest and most rapid changes in blood pressure. The elastic membranes or laminae are separated from each other by smooth muscle fibers, fibroblasts, and collagenous and reticular connective tissue fibers. Note that the elastic laminae are unstained by the methods used here.
Collagen: Primarily located external to the outermost elastic lamina, it stains a bright blue with Mallory and Mallory-azan stains. Note the collagenous connective tissue immediately adjacent to the elastic laminae. The methods used here selectively stain collagenous fibers
Lymph node
subcapsular sinus
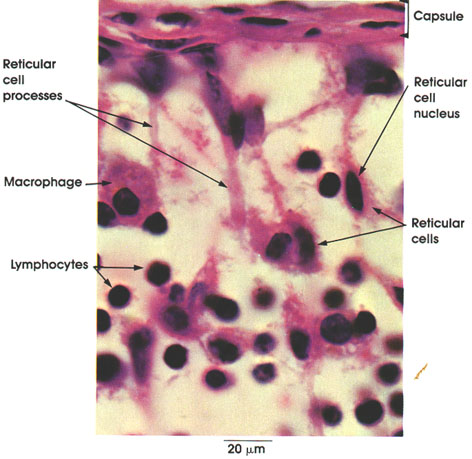
The subcapsular sinus of a lymph node is a lymph channel beneath the capsule of the node . The component elements of the sinus are seen in this figure: reticular cells and their processes, which form a meshwork. Reticular cells are "star-shaped," with lightly staining cytoplasm and processes that are in contact but not continuous with processes of adjacent cells. These stellate reticular cells and their processes form the reticular tissue meshwork of the node in which lymphocytes and free macrophages are found.
Liver
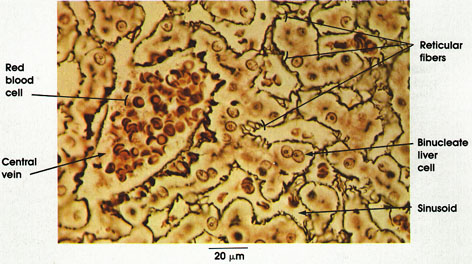
Reticular fibers: Reticular fibers branch and anastomose in a delicate fibrous network delineating the sinusoids. They are of small diameter and are resistant to dyes, making them difficult to demonstrate except by special techniques such as the method used in this preparation.
Binucleate liver cells: These are polyhedral cells with centrally placed nuclei and prominent nucleoli. Occasionally, they are multinucleate.
Sinusoids: Sinusoids constitute the intralobular system of specialized vascular channels. They carry blood from interlobular branches of the portal vein centripetally to the central vein. They anastomose and separate adjacent hepatic cellular plates.
Central vein: This is located in the center of the hepatic lobule. It is the smallest radicle of hepatic veins and receives the contents of all the sinusoids of the hepatic lobule.
Red blood cells: Filling the central vein, they carry oxygen to the hepatic cells and remove carbon dioxide. The red blood cell is approximately 6 µm in diameter and can be used as a rough internal measure.
Duodenum smooth muscle
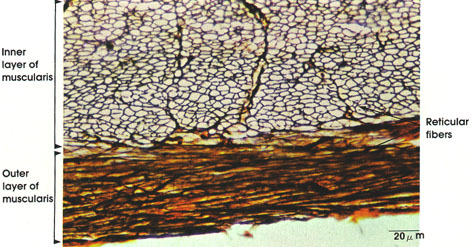
This is part of the muscular coat of the duodenum, stained with a special silver technique to demonstrate reticular fibers. Note the abundance of reticular fibers between muscle fibers. The latter are not stained by this method. The negative outlines of the transversely sectioned muscle fibers of the inner circular coat are well delineated by the stained reticular fibers.
Mediastinum
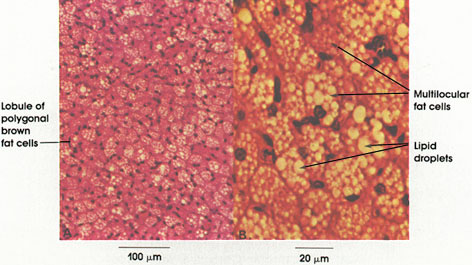
Brown fat is an uncommon variety of human fat found in the upper back (interscapular region) of the body. Unlike the more common white fat, brown fat cells contain a number of small lipid droplets, hence the name multilocular fat. White fat cells, in contrast, contain a single lipid droplet
Panniculus adiposus
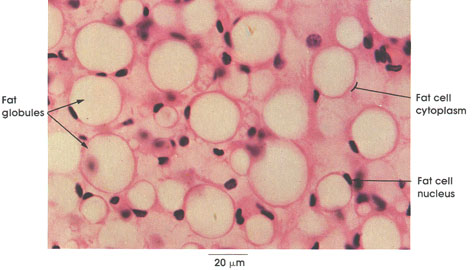
The fat cell lipid is in the form of a single droplet, and these cells are described as unilocular. In brown fat .the lipid appears as small multiple droplets, and these cells are described as multilocular.
Fat cell cytoplasm: This appears as a thin rim at the periphery of the cell. Stored fat is the predominant component of cytoplasm.
Fat cell nucleus: The nucleus is flattened in the cytoplasm, permitting maximum storage of fat globules.
Fat globules: These appear as empty spaces because the fat has been dissolved out by solvents used in the preparation of tissues. Special fixatives and stains are needed to demonstrate lipid droplets .At body temperature, the fat is liquid.
Trachea
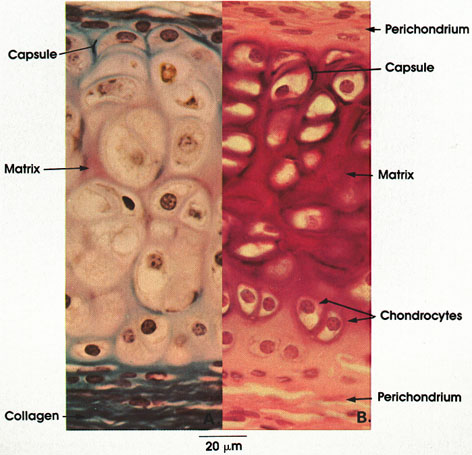
B. Rat, Helly's fluid, toluidine blue and erythrosin, 612 x.
Perichondrium: A dense layer of irregular fibrous connective tissue that always invests hyaline cartilage except at the free surfaces of articular cartilage. Note how the perichondrium in A is better shown by a connective tissue stain (Mallory's) specific for collagen.
Chondrocytes: Two or more cartilage cells enclosed within smooth-walled spaces or lacunae. Note the centrally placed, large spherical nuclei (isogenous grouping). The vacuolation noted in the cytoplasm of chondrocytes is an artifact of processing resulting from poor preservation of fat droplets and glycogen. Note the rounded appearance of chondrocytes centrally located and the flattened appearance of cells near the perichondrium.
Matrix: Derived from a Latin word meaning womb, matrix is a place where something is formed and a medium enclosing other bodies. The matrix is composed of ground substance (protein polysaccharicle) and connective tissue fibers. It fills the space between chondrocytes. In B, note the metachromasia of the matrix stained with toluidine blue. The metachromasia is due to the high content of chondroitin sulfate.
Capsule: The walls of the lacunae are referred to as a capsule. The capsule is a condensation of the matrix surrounding the lacunae.
Epiglottis
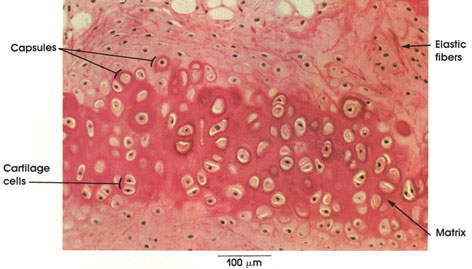
Cartilage cells: These cells are large and pleomorphic and are housed in lacunae of the matrix. One or more cells may be found in one lacuna.
Capsules: Condensed matrix surrounding cartilage cells. These capsules stain intensely and represent the most recent deposition of matrix.
Matrix: The matrix contains collagenous and elastic fibers embedded in a highly acidic ground substance consisting of chondroitin sulfate and protein.
Elastic fibers: Oriented in all directions within the matrix, elastic fibers give flexibility to the cartilage.
Finger phalanx
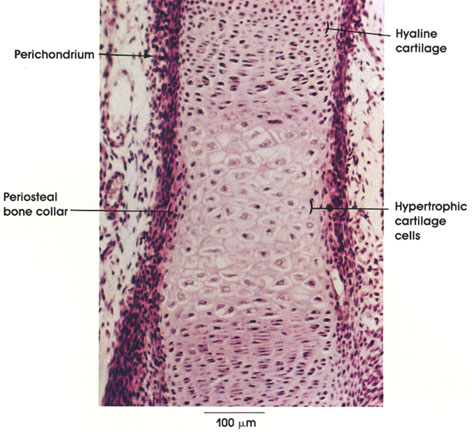
Endochondral bone is a form of ossification in which an embryonal type of hyaline cartilage precedes the formation of bone. In this figure, note the change from the zone of reserve cartilage cells to the zone of hypertrophic cartilage cells. Lacunae are increased in size, and the interlacunar space is reduced in the region of the hypertrophic cells. Note the concomitant change in the perichondrium in which the inner cells change into osteogenic cells (osteoblasts) leading to the formation of the periosteal (perichondral) bone collar.
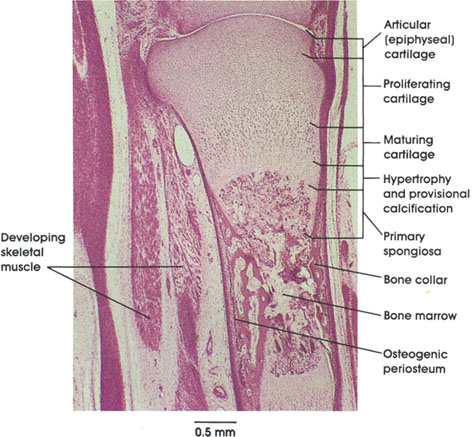
Detail from a later stage of bone formation in which a bony collar has formed and cartilage is undergoing various bone growth-related changes. The development of a bone collar initiates the hypertrophy of cartilage cells. This is followed by a vascular intrusion into the cartilaginous core bringing along with it osteoblasts and chondroclasts from the osteogenic connective tissue perichondrium. The osteogenic cells lay down osseous tissue internally and the bony collar expands, in the long axis distally, in both directions. The structural components of the cartilage at this stage have been identified as (1) so-called resting, epiphyseal, or articular cartilage, which is adjacent to (2) proliferating cartilage, which is characterized by mitotic figures and flattened chondrocytes, which synthesize and secrete matrix. The next zone (3) is named maturing cartilage, where matrix is also synthesized and presumably prepared for calcification. The cells enlarge and accumulate glycogen; then the cells become inactive and vacuolated and the nuclei pyknotic, after which they die. This region is known as (4) the zone of hypertrophy. When the lacunae housing chondrocytes break down in the transverse plane, they form spicules of cartilage, which become calcified, resulting in the formation of (5) the so-called primary spongiosa into which capillary loops advance. The advancing blood vessels bring in osteogenic cells, which continue the calcification process and development of bone.
The formation of a mature bone involves the following developmental stages: (1) intramembranous ossification, (2) endochondral ossification, (3) growth, (4) shaping or modeling to desired shape, and (5) remodeling mature bone over time.
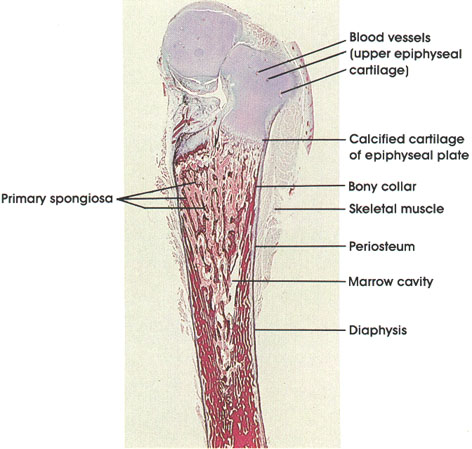
At this stage of development, the upper epiphyseal cartilage has been invaded by blood vessels and mesenchyme prior to the formation of the epiphyseal ossification center.
The diaphyseal bony collar extends to the epiphyseal plate composed of calcified cartilage. The formation and remodeling of the diaphysis can be seen to be well advanced.
The process of bone formation will not be complete, and bone growth ended, until the epiphyseal plate disappears and the marrow cavity becomes continuous throughout the bone. The blood vessels of the diaphysis, epiphyses, and metaphyses will then intercommunicate.
MEMBRANE BONE
Mandible
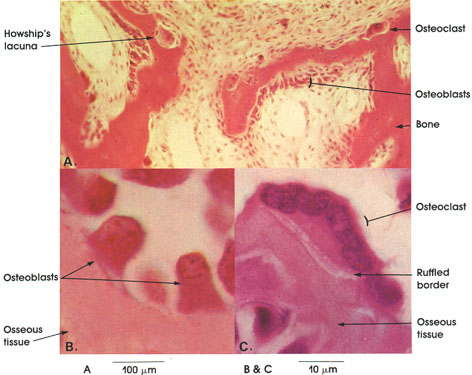
Cat, Müller's* fluid, H. & E., A. 162 x; B. & C. 1416 x.
0steoclast: A multinucleated giant cell associated with areas of bone resorption. The surface adjacent to bone being resorbed has numerous cytoplasmic processes, giving the ruffled border appearance.
Osteoblasts: Responsible for bone matrix formation and present wherever osseous tissue is elaborated. In membranous bone, osteoblasts arise as differentiated mesenchymal cells.
AND FIBROCARTILAGE
Tibia knee joint
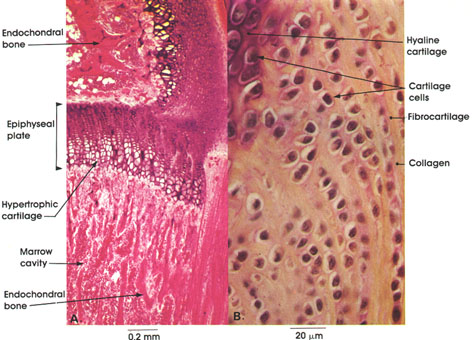
B. Gomori's aldehyde fuchsin, 612 x.
Enclochondral bone formation is a process in which an embryonal type of hyaline cartilage precedes bone formation. In A, a stage in the endochondral ossification in a long bone (tibia) is shown. Note the cartilaginous epiphyseal plate that separates the epiphysis (above) from the diaphysis (below). The epiphyseal plate is the source of new cartilage, which is replaced by bone during growth in length. Note the zone of hypertrophic cartilage within the epiphyseal plate. This is a stage in endochondral bone formation preceding calcification. Islands of formed endochondral bone are seen above and below the epiphyseal plate in the epiphysis and diaphysis. Note the marrow cavity between plates of endochrondral bone in the diaphysis. This cavity is formed by resorption of endochondral bone.
In B, note the characteristic grouping of fibrocartilage cells and their arrangement in rows separated by dense collagenous connective tissue. Adjacent to fibrocartilage, note the hyaline cartilage cells.
Fibula

Haversian canal: Conducts blood vessels, lymphatics, and nerves through bone. Haversian canals surrounded by concentric lamellae of compact bone form the Haversian system. These canals are named after Clopton Havers, an English physician, who described them in his Osteologia Novia, published in London in 1691.
Blood pigment: From disintegrated blood elements in the vessels within the Haversian canals.
Lacunae and canalicull: The former are cell spaces that housed osteocytes, and the latter are channels extending out of the lacunae that accommodated cell processes of osteocytes.
Compact cross section
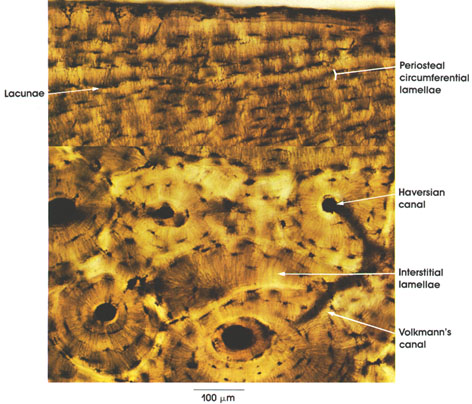
Haversian canals: These are abundant and characteristic of compact bone. Their course follows the main axis of long bone. They conduct blood vessels, lymphatics, and nerves throughout the bone. They branch and anastomose and become continuous with Volkmann's canals. Haversian* canals surrounded by concentric lamellae of compact bone form the Haversian system.
Volkmann's canals: These are cross connections between Haversian canals. They pierce the lamellae of two Haversian systems. They contain blood vessels, lymphatics, and nerves and supply the interstitial lamellae.
Interstitial lamellae: A set of bone lamellae that fill the spaces between Haversian systems. They vary in shape and orientation
Fetal pig
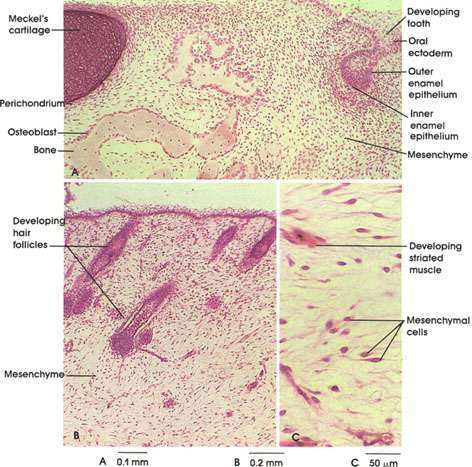
Mesenchymal connective tissue has a delicate spongy consistency and is composed of cells and a viscous matrix or ground substance containing few fibers.
Mesenchymal cells are characterized by oval elongate nuclei with prominent nucleoli and a mix of hetero- and euchromatin. These cells have little cytoplasm but many thin processes that appear to extend from the nucleus. Mesenchymal cells can differentiate into most of the adult connective tissue cell types, including: (1) fibroblasts, (2) chondroblasts, (3) osteoblasts, (4) odontoblasts, (5) reticular cells, and (6) adipocytes.
The matrix is composed of two classes of compounds: glycosaminoglycans and structural glycoproteins.
In this plate, note several of the mature cell types that have differentiated from mesenchymal cells. Examine the developing tooth in A and the developing hair follicles in B.
MUCOUS CONNECTIVE TISSUE
Umbilical cord
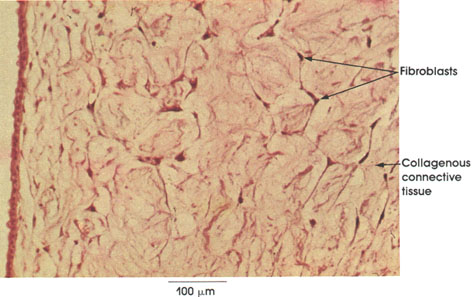
Rhesus monkey, Helly's fluid, H. & E., 162 x.
Mucous connective tissue is characteristically found in the umbilical cord. It also is transiently encountered as a stage in the differentiation of mesenchyme into connective tissue.
The distinctive cell of mucous connective tissue is a primitive fibroblast, which may be spindle-shaped or stellate. In H. & E. preparations, only nuclei of fibroblasts are evident. Fine collagenous fibrils aggregate in the ground substance, which is characteristically abundant and gelatinous.