Section 12: Urinary System
The urinary system consists of the kidneys, ureters, urinary bladder, and urethra.
The volume and composition of body fluids are maintained remarkably constant regardless of fluid and solute intake. The regulation of body fluid and the constancy of the internal environment is the primary role of the kidneys.
Each kidney resembles the bean of the same name. At the center of the concave side, where the ureters and veins issue and arterial vessels and nerves usually enter, is the hilus. The kidneys are covered by a dense collagenous capsule called the renal capsule. The organ has a cortex and an inner medulla. The cortical area is clearly defined from the inverted conical or pyramid-shaped medulla. The base and sides are surrounded by cortical tissue, and the apex protrudes into the renal calyces. These protrusions are called renal papillae, whose surface is perforated by openings of numerous papillary ducts (of Bellini) and is thus called the area cribrosa.
From the base of the medullary pyramid, several hundred elongated parallel arrays of tubules enter the cortex. These so-called medullary rays consist of individual units composed of a straight collecting duct surrounded by many parallel tubular parts of the nephron. A renal lobule is defined as a single medullary ray and the cortical tissue that surrounds it. The cortical tissue in the area between the medullary pyramids constitutes the renal columns of Bertin. The cortex is punctuated by many renal or Malpighian corpuscles. The renal cortex consists of nephrons and blood vessels.
The human kidney has about four million filtering units called nephrons. The nephron consists of four parts: (1) renal corpuscle (capillary loops surrounded by an epithelial cover), (2) proximal convoluted tubule, (3) thin and thick limbs of Henle, and (4) distal convoluted tubule. The components of the nephron are completely covered by a basal lamina. The renal corpuscle is composed of two parts: a "tuft" of capillaries and a double-walled epithelial capsule called Bowman's capsule. The interior of Bowman's capsule (Bowman's space) is continuous with the proximal convoluted tubule.
Every minute, approximately one fourth of the cardiac output of blood enters the kidneys, and all the circulating blood passes through the kidneys every 5 minutes. The blood flows through the glomerular capillaries under 45 mm Hg pressure, and about one fifth of the plasma water leaves the capillaries and enters Bowman's space and the proximal tubules. The blood remaining in the capillaries flows into the efferent arterioles, which break up into capillary peritubular networks closely applied to renal tubules.
Plasma water in Bowman's space is termed the glomerular filtrate and normally contains all the major ions, amino acids, glucose, urea, and other substances in approximately the same concentration that exists in the blood plasma. However, this ultrafiltrate does not normally contain red blood corpuscles or significant amounts of protein. Both water and solutes are reabsorbed across the renal tubule cells to the fluid-filled interstitial space and into the peritubular capillaries to reenter the blood stream. This is called tubular reabsorption. Other substances leave the peritubular capillaries, enter the interstitial fluid, and are transported across the tubule cells, where they enter the tubule to be added to the glomerular filtrate. This is called tubular secretion.
The proximal convoluted tubule reabsorbs the filtered glucose and amino acids and some of the sodium, chloride, and bicarbonate ions. This active process, enhanced by the numerous microvilli that increase the surface area of proximal tubule cells, results in an osmotic gradient, which causes the passive reabsorption of water. The content of the proximal tubule is isotonic with respect to the blood plasma. The distal straight portion of the proximal tubule is in continuity with the thin limb of the loop of Henle, which extends into the kidney medulla and returns as the thick limb to the cortex. The content of the descending thin limb becomes increasingly hypertonic as salt (active chloride pump) is actively transported from the ascending limb into the interstitial space surrounding the descending thin limb. Chloride, together with sodium ions, passively enters the descending limbs, as water is drawn to the interstitium. Unlike the descending limb, the ascending limb of the loop of Henle is impermeable to water, and the content of the ascending limb of the tubule becomes increasingly hypotonic as salt is actively transported from it. Sodium ions are actively reabsorbed, and water is passively reabsorbed in the distal tubule.
The ascending thin limb of the loop is in continuity with the distal tubule. The distal tubule and the collecting duct are engaged primarily in the regulation of acid-base and potassium ion balance in the blood. Sodium ions are conserved (under the influence of the hormone, aldosterone) and exchanged for hydrogen or potassium ion, or both. The distal convoluted tubule cells do not have numerous microvilli but rather are characterized by infoldings of their basal cell membrane forming compartments containing mitochondria. These result in the appearance in light microscopy of so-called basal striations. These cellular architectural modifications facilitate active transport between the interstitial fluid and the lumen of the distal tubule.
The final concentration of urine, by passive reabsorption of water to form a hypertonic urine, occurs in the collecting ducts as they pass through the region of increasing osmolality in the medulla produced by the thin loop of Henle. This is facilitated by the action of antidiuretic hormone on the membrane permeability of the cells lining the collecting ducts. The urine leaves the kidney via papillary ducts, enters the ureter, and is stored'in the urinary bladder. Contraction of the urinary bladder forces the urine into the urethra to be eliminated from the body. A single kidney produces roughly 63 ml of glomerular filtrate per minute and reabsorbs 62 ml. Hence, 1 ml is drained into the bladder as urine, resulting in an output of 1440 ml per 24 hours.
The kidneys are also the site of synthesis of the hormone renin. Adjacent to the renal corpuscle and distal convoluted tubule, the internal elastic lamina of the afferent arteriole disappears and the smooth muscle cells become structurally modified (epithelioid in appearance) and synthesize and store the hormone renin in the form of granules. These granules stain intensely with periodic acid-Schiff method and also following Zenker's fixation with several common histologic dyes. These cells are called juxtaglomerular (JG) cells. The distal tubule cells immediately adjacent to JG cells are also modified, appearing with tightly packed nuclei, and the area is called the macula densa. The macula densa and JG cells are jointly called the juxtaglomerular apparatus. In addition to the juxtaglomerular apparatus, there are some pale staining cells of unknown function associated with afferent arterioles that are variously given several names, including extraglomerular mesangial, lacis, or polkissen cells. Anything that results in a reduction of blood flow to the kidney, such as an aneurysm or significant blood loss, will activate the secretion of stored renin. Renin acts on a plasma protein termed angiotensinogen, resulting in the formation of an inactive decapeptide, angiotensin I. In the presence of a converting enzyme (found in high concentration in lung endothelium), angiotensin I becomes an octapeptide termed angiotensin II. Angiotensin II is a powerful vasoconstrictor. It also causes enhanced secretion of the adrenal cortical hormone, aldosterone, which acts on the cells of distal tubules to increase the reabsorption of sodium and chloride ions. This, in effect, increases blood pressure by increasing the volume of extravascular fluid. Chronic deficiency in blood flow to the kidneys can result in a serious, life-threatening hypertension.
Some names associated with the urinary system follow: Bellini was a seventeenth -century Italian anatomist; Bertin, an eighteen th-century French anatomist, Malpighi, a seventeen th-century Italian anatomist, Henle, a nineteenth-century German anatomist; Bowman, a nineteenth-century English anatomist; Schiff, a twentieth-century German chemist in Florence, and Zenker, a nineteenth-century German pathologist
Fetal
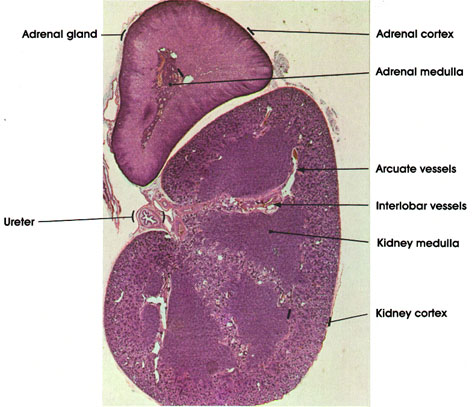
In this plate, the gross histologic features of the adrenal gland and the kidney are seen. Note the location of the adrenal gland, riding the superior pole of the kidney. Within the kidney, note the hilum where the ureter is seen in cross section and where vessels are seen entering and leaving the kidney. The divisions of the kidney into cortex and medulla are clearly seen. Note the peripheral location of the cortex and the cortical columns that dip between the medullary pyramids. The latter are pyramid-shaped medullary structures, with the base of the pyramid resting against the peripheral cortex and the apex toward the hilum. Between the pyramids, note the interlobar vessels. The interlobar artery is a branch of the renal artery. The interlobar veins form the renal vein. in the marginal zone, between the cortex and base of the pyramids, course the arcuate arteries and veins, which are tributaries of the interlobar vessels.
In the adrenal gland, note the subdivisions into cortex and medulla
Cortex
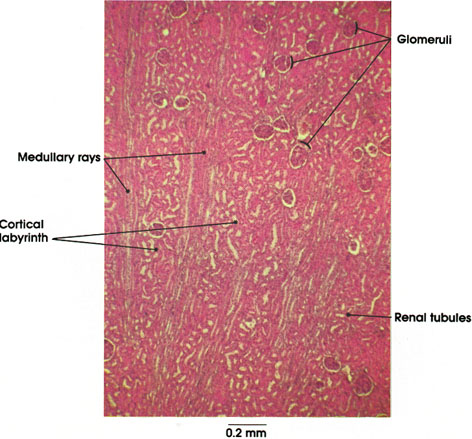
In this plate, the various constituents of kidney cortex are shown. The cortex is composed of radiating columns of straight renal tubules (medullary rays), alternating with regions containing glomeruli and convoluted renal tubules (cortical labyrinth). Other names for these two divisions are pars radiata or the processes of Ferrein* for the medullary rays, and the pars convoluta for the cortical labyrinth. The cortical labyrinths contain glomeruli, proximal and distal convoluted tubules, and the arched collecting tubules. The medullary rays contain the straight portions of proximal tubules (medullary segments), the thick segments of ascending arms of Henle's* loops, and the straight collecting tubules.
Vascular system cortex
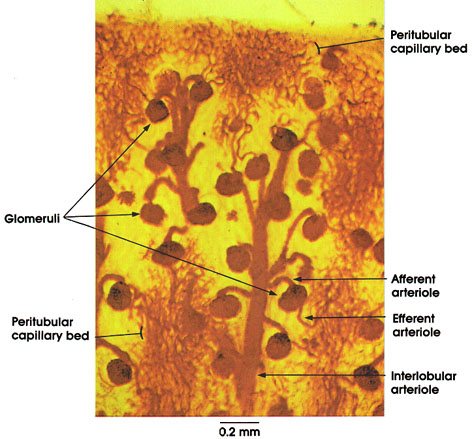
This is an injected specimen to demonstrate some aspects of vascular supply of the kidney. The interlobular arteries are branches of the arcuate arteries. The latter are located in the zone separating the cortex from the base of the medullary pyramids. The interlobular arteries ascend perpendicularly to the surface of the kidney and provide numerous short lateral branches (afferent arterioles) that enter one or more renal corpuscles (glomeruli). The interlobular arteries terminate at the periphery of the cortex as afferent arterioles, and each supplies a glomerulus. From every glomerulus, an efferent arteriole leaves and divides into a system of capillaries called the peritubular plexus around the tubules of the cortex. The injected carmine gelatin illustrates the larger size of the lumen of afferent arterioles. This relative size difference presumably increases the glomerular filtration pressure.
Cortex
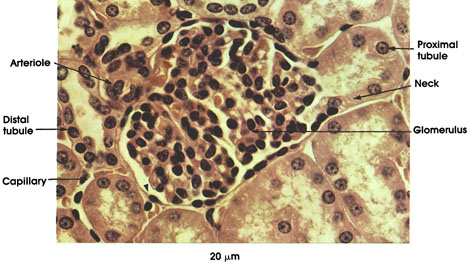
Proximal tubule: Lumen continuous with that of glomerular capsule (Bowman's space). Large cuboidal cells, abundant eosinophilic cytoplasm, and large spheroidal nuclei. Brush border.
Neck: The first part of the proximal tubule leading away from the glomerulus. Narrow and straight.
Distal tubule: Wider lumen, shorter cells, without brush border.
Glomerulus: A tuft of winding capillaries surrounded by epithelial cells and few connective tissue cells.
Arteriole: Afferent arteriole breaks up into many capillary loops inside the glomerulus. From these capillaries, the efferent arteriole is formed.
Capillary: Surrounds the renal tubules. These capillaries are branches of the efferent arteriole
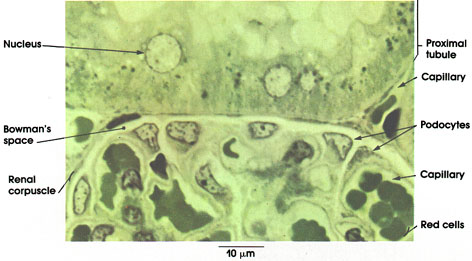
Proximal tubule: Single layer of cuboidal cells with irregular surface. Rounded nucleus. Granular cytoplasm (see also Plate 16).
Capillary: Within the renal corpuscle. Filled with red blood cells.
Podocytes: The name given to cells of the visceral epithelium of Bowman's capsule. They have many foot- like processes (podia) resting upon the basement membrane covering the capillaries.
Bowman's space: Space between the parietal and visceral layers of Bowman's capsule in continuity with the lumen of the proximal tubules. .
Renal corpuscle: Includes Bowman's capsule plus the glomerulus formed of capillaries. Also known as Malpighian body
Cortex
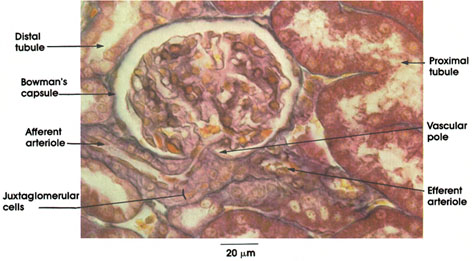
Bowman's capsule: Squamous epithelium forming a double-walled cup surrounding the glomerular capillaries. The portion of the wall applied to the capillaries is termed the visceral epithelium . The visceral epithelium is separated from the outer wall by Bowman's space .The outer wall is continuous with the proximal tubule, and Bowman's space is continuous with the lumen of the proximal tubule at the urinary pole of the capsule.
Vascular pole: The point of entry of the afferent arteriole into Bowman's capsule. The arteriole immediately forms the tuft of glomerular capillaries and the point of origin of the efferent arteriole from glomerular capillaries, which leaves Bowman's capsule.
Afferent arteriole: Carries blood to the glomerular capillaries.
Efferent arteriole: The arterial vessel that carries blood away from the glomerular capillaries. Uniquely, in the kidney, a capillary bed is interposed between arterial vessels. The efferent arteriole leads to the cortical intertubular capillary network
Juxtaglomerular cells: Myoepithelioid cells replace typical smooth fibers in the wall of the afferent arteriole as it approaches the glomerulus. These cells secrete a hypertensive factor, renin. .
Proximal tubule: Single layer of cuboidal cells with an irregular brush border.
Distal tubule: Cuboidal cells without a brush border, which stain less intensely than the proximal tubule cells.
Cortex
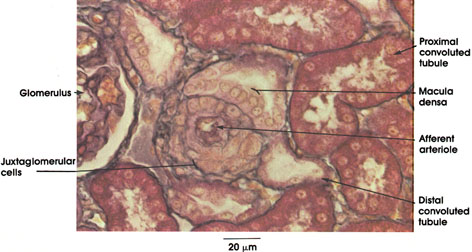
Afferent arteriole: Seen here in cross section. Its proximity to the glomerulus (not seen here), which it serves, is indicated by the presence of cells containing conspicuous granules, which replace smooth muscle fibers normally found in the wall of arterioles.
Juxtaglomerular cells: Rich in cytoplasmic granules containing renin. Renin secreted into the blood is known to play a role in the formation of a hypertensive substance known as angiotensin II.
Glomerulus: Tuft of capillaries having their origin from the afferent arteriole and surrounded by Bowman's capsule. The glomerulus, together with Bowman's capsule, constitutes the renal corpuscle.
Proximal convoluted tubule: Outlet of Bowman's capsule approximately 14 mm long with many small loops near the renal corpuscle. It ultimately straightens and runs toward the medulla in the medullary rays.
Distal convoluted tubule: This portion of the renal tubule has many short loops in close association with the proximal convoluted tubule and the glomerulus. It is about one third the length of the proximal tubule. The distal tubule is continuous with the collecting tubules.
Macula densa: Specialized region of the distal convoluted tubule with tightly packed tubule cells in contact with the afferent arteriole. The bases of the cells of the macula densa are consistently found in intimate association with the juxtaglomerular cells in the wall of the afferent arteriole. Because this structural relationship suggests a functional relationship (supported experimentally), the macula densa and the juxtaglomerular cells together are referred to as the juxtaglomerular apparatus.
Juxtaglomerular cells
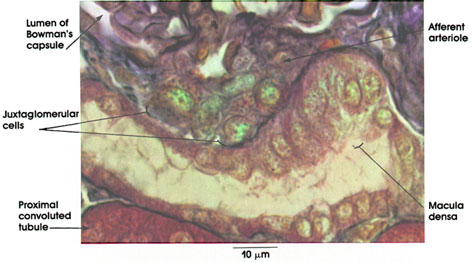
Afferent arteriole: Terminal branch of the interlobular artery entering the glomerulus. The renal afferent arterioles are volume receptors and are sensitive to changes in perfusion (blood) pressure.
Juxtaglomerular cells: Granular variety of myoepithelioid cells in the wall of the afferent arteriole. Replace the typical smooth muscle cells of the tunica media of the artery. A decrease in afferent arterial volume secondary to low perfusion pressure results in the release of renin. Renin is an enzyme that is released into the blood and acts upon blood proteins to produce a potent vasoconstrictor, angiotensin, which can, under abnormal conditions, elevate blood pressure to dangerous levels. Hypertension of renal origin in humans can be cured by removal of the diseased or ischemic kidney. Renin also affects blood volume and osmolarity by initiating a chain of events leading to the release of the hormone aldosterone by the cells of the zona glomerulosa of the adrenal cortex. Aldosterone acts upon the renal tubules to enhance sodium reabsorption. A second system unrelated to the kidney (the hypothalamus of the brain and the posterior lobe of the pituitary, neurohypophysis), also regulates the volume and osmolarity of the extracellular fluid of the body.
Macula densa: A group of specialized cells of the straight portion of the distal tubule, in contact with the afferent arteriole and contiguous with the juxtaglomerular cells. The cells are taller, thinner, and tightly packed compared to other distal tubule cells. These cells are functionally related to the juxtaglomerular cells, although their exact role is undefined. The macula densa marks the origin of the convoluted portion of the distal tubule.
Lumen of Bowman's capsule: Located between the parietal and visceral epithelial layers. Receives the ultrafiltrate of blood plasma circulating through the glomerular capillaries. The glomerular filtrate traverses the glomerular endothelium, the basal lamina (basement membrane), and the visceral epithelium to reach Bowman's space. Bowman's space is continuous with the lumen of the proximal convoluted tubule.
Proximal convoluted tubule: Deeply staining cuboidal cells surrounded by a thin basal lamina (basement membrane).
Medulla
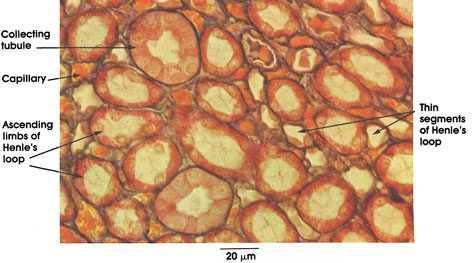
Collecting tubule: Cuboidal or columnar lining. Nuclei round and dark. Cytoplasm clear with distinct cell outlines.
Capillary: Filled with red cells.
Ascending limb of Henle's loop: Lined by cuboidal cells.
Thin segments of Henle's loop: Cells flattened, single layer, nuclei bulge into lumen.
Papilla, area cribrosa, minor calyx
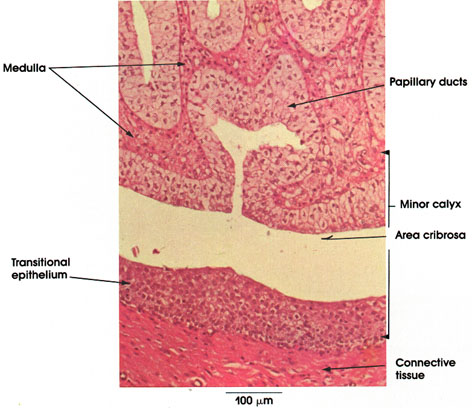
Papillary ducts (of Bellini): Named after Lorenz Bellini, the Italian anatomist, who described them in 1662. Arise by convergence of collecting tubules in the medulla near the pelvis. These ducts have large lumina and open at the area cribrosa at the apex of the papilla. Note the tall columnar epithelium lining the ducts. Cytoplasm of epithelial cells is clear; nuclei are dark and basally located. The tops of cells tend to bulge into the lumen.
Minor calyx: Subdivision of a major calyx in the pelvis of the kidney. The minor calyx is an infolded tube forming a double-walled cup. The inner wall of the calyx fits over the papilla of a pyramid. The transitional epithelium of the minor calyx is continuous with the columnar epithelium of the papillary ducts. The lamina propria is made up mostly of collagenous connective tissue and lacks papillae.
Area cribrosa: The sieve-like appearance of the papilla is produced by the large number of collecting tubules passing through it.
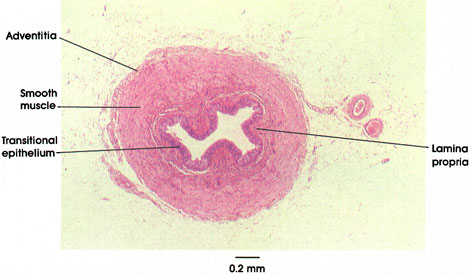
In cross section, the ureter typically exhibits a "festooned" appearance, reflecting contraction of the thick surrounding muscular layer and the consequent development of deep mucosal folds, consisting of the transitional epithelium and underlying lamina propria. There is no submucosa-the tissue of the lamina propria blends with the epimysial connective tissue of the muscularis. As in other urinary passages, the muscular layers are defined as inner longitudinal and outer circular (the converse of the gastrointestinal tract). However, these are not consistently clearly demarcated in histological section owing to incomplete separation of layers and intermingling of muscle fibers. The well-developed muscular layer generates the vigorous peristaltic wave, which propels urine from the renal pelvis to the urinary bladder. At the site of entry of the ureters into the bladder (the intramural portion of the ureter), the circular muscle layer disappears, and the ureters run an oblique course through the bladder wall. This anatomical arrangement, together with the closing of a fold of the bladder mucosa over the orifice of the ureter by hydrostatic backpressure of the bladder contents, provides an effective "physiological valve," which prevents backflow (reflux) of urine from the bladder to the ureter, and subsequently to the kidney pelvis. These anatomical features ensure against the kidney's being subject to hydrostatic pressure and tissue damage (hydronephrosis) upon voiding, and prevents reflux of bladder urine and transmission of infection to the upper urinary tract.
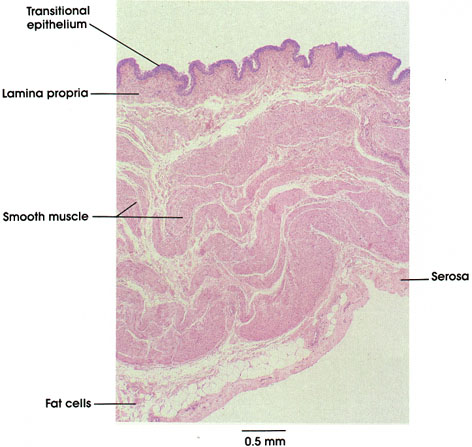
The component parts of the wall of the urinary bladder are shown at low power. The innermost layer, the mucosa, consists of transitional epithelium, underlaid by a prominent lamina propria. The folds in the mucosa are seen in three dimension to be extensive longitudinal ridges and represent one means by which the bladder wall accommodates to distention. The thickness of the epithelium is also reduced upon stretching, as is the height of the luminal epithelial cells (dome, or umbrella cells, see Plate 24 for details of the epithelium). Thus, the overall topography of sections of the bladder will always depend upon the state of distention and turgidity of the organ at the time of fixation. The muscular layer of the bladder is generally recognized as consisting of three layers: (1) inner longitudinal, (2) middle circular or spiral; and (3) outer longitudinal. The definition of these as discrete layers is rendered difficult by the intertwining of muscle bundles and fascicles from adjacent layers, and by variation in the thickness of the respective layers in different parts of the organ (e.g., the formation of the internal sphincter by the internal longitudinal layer in the region of the trigone). This histological feature is in contradistinction to the well-defined muscle layers evident in preparations of the gastrointestinal tract. Such a muscular arrangement does, however, facilitate the occlusion of the bladder lumen upon voiding, and the avoidance of residual urine in the bladder, which is recognized as predisposing to bladder infections. The organ is covered by a connective tissue adventitia, except on its superior aspect, which bears a serosa of reflected peritoneum. Present within this layer are blood vessels, nerves, and underlying adipose tissue.
Female
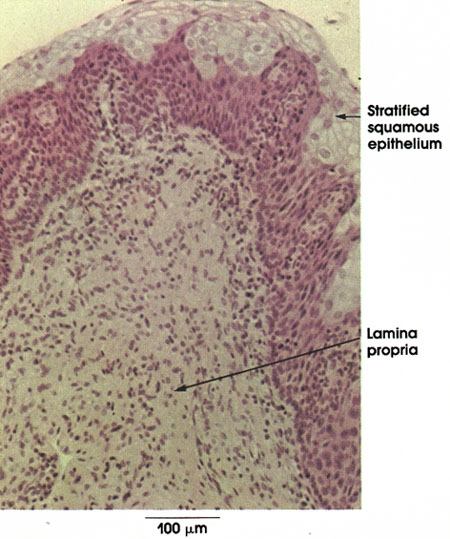
This is a section of female urethra showing the mucosa. The lining epithelium here is stratified squamous. The type of epithelium lining the urethra is variable at different sites. It is transitional near the urinary bladder and stratified squamous throughout most of its extent except for interrupted segments of stratified columnar or pseudostratified epithelium. The lamina propria of loose connective tissue lacks papillae.
Cavernous portion
penis
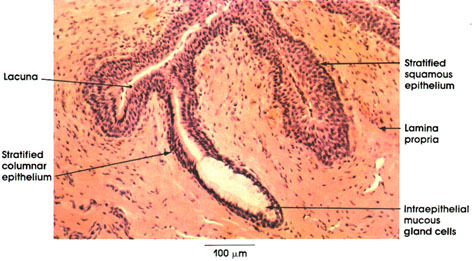
This plate shows the histology of the Cavernous portion of the male urethra. This portion of the urethra extends throughout the penis to open at the end of the glans. Note the stratified columnar epithelium mucosal lining intermixed with stratified squamous epithelium. The latter type of epithelium is found in interrupted areas throughout the extent of the urethra and is the only epithelial type found at the external opening of the urethra.
Note the deep recesses of the mucosal surface known as lacunae of Morgagni* Isolated intraepithelial mucous gland cells are seen interspersed between the stratified columnar cells lining the lacunae.
The lamina propria is made up of loose connective tissue rich in elastic fibers.